BEDRIDDEN OVERNIGHT.
IMAGINE YOU GET THE FLU AND THEN NEVER GET OUT OF BED AGAIN.

Myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS)
A characteristic feature of ME/CFS is post-exertional malaise (PEM), in which symptoms worsen after physical or mental exertion (leading to a so-called collapse). In severe cases, even minimal activities such as taking a shower, walking a few steps or even turning over in bed can be enough to trigger a collapse.
The disease is also characterized by a wide range of other symptoms that can change over time and vary from person to person. Patients may suffer from persistent fatigue, unrefreshing sleep, profound weakness, problems with thinking and concentration (brain fog), orthostatic intolerance, pain and many other symptoms.

How many people are affected?
- In Austria, an estimated 60,000 to 80,000 people are affected, mainly young adults.
- More than 40 million people worldwide live with the disease, around 75% of whom are women.
- The disease often occurs after infections, for example with the Epstein-Barr virus or COVID-19.

Severity
- Around 25% of those affected are homebound, with severe cases even bedridden and dependent on 24-hour care.
- 60 to 70 percent are unable to work.
- Stimuli such as light, noise or touch can significantly worsen the symptoms.
The severity and disease burden of ME/CFS
The severity of the symptoms varies greatly from patient to patient and can also fluctuate over time in individual cases. However, even “mild” sufferers are considerably restricted in their everyday lives. They need longer periods of rest every day, are unable to perform strenuous physical activities and therefore have difficulty holding down a regular job or attending school. Around 25% of patients with severe ME/CFS are housebound and dependent on the help of others.
Even basic activities such as preparing meals or doing the laundry become difficult. Due to sensory overload, communication with friends and family or online activities are only possible for a short time each day. Finally, people with very severe ME/CFS are bedridden, unable to meet even their most basic needs and dependent on 24-hour care. Conversation is impossible, and they often find themselves isolated in dimly lit rooms, surrounded by absolute silence, as any stimulation can trigger post-exertional malaise (PEM).
Due to the high severity, chronic nature of the disease and its considerable prevalence, the global disease burden of ME/CFS is high and has been shown to be twice that of HIV/AIDS and more than half that of breast cancer. However, an examination of resource allocation in relation to disease burden reveals that ME/CFS is dramatically underfunded. Compared to the NIH’s analysis of funding allocation, ME/CFS receives only about 7% of the funding that would be commensurate with its disease burden. This underscores the need for increased attention and support for ME/CFS research and care.


Disease pathology, therapy and prognosis
Due to the heterogeneity of the disease and decades of under-research, the pathology of ME/CFS remains poorly understood. Although many studies show pathophysiological abnormalities, e.g. in energy metabolism, the immune system and the vascular system, there is no validated biomarker that can be used for diagnosis.
There is no FDA or EMA approved treatment and no cure for ME/CFS. Apart from symptomatic treatment (e.g. for sleep disorders or pain), the most important recommendation for patients is pacing, i.e. adherence to individual stress limits imposed by the disease through activity and energy management.
The aim is to avoid relapses due to post-exertional malaise and to create optimal conditions for stabilization of the disease. However, the long-term prognosis remains poor. Although a gradual improvement is sometimes observed, the rate of complete remission is less than 5%.

Designations for ME/CFS
Over the years, the disease has been referred to by various names, each with its own historical context, geographical background, stigma and burden. The most commonly used names are myalgic encephalomyelitis (ME) and chronic fatigue syndrome (CFS). The World Health Organization classifies both ME and CFS as neurological disorders under the same ICD-10 code G93.3. In recent years, however, the combined term ME/CFS has become increasingly established in the scientific literature and has been adopted by healthcare providers, professionals and patient organizations. In line with this emerging consensus, we use the technical term ME/CFS for the disease – without prejudice to the disease pathology.

Symptoms and concomitant diseases
ME/CFS is a multi-system disease with symptoms affecting almost every part of the body. Although their expression and relative severity may vary from person to person, the combination of symptoms is characteristic and allows diagnosis by an experienced clinician according to international guidelines. Modern criteria considered appropriate for both clinical diagnosis and research case definition include the Canadian Consensus Criteria (CCC) and the International Consensus Criteria (ICC).
Post-exertional malaise (PEM):
A characteristic feature of ME/CFS is the worsening of symptoms after even minimal physical or cognitive exertion. This post-exertional malaise can lead to a prolonged period of increased fatigue, brain fog and other symptoms, also known as a “crash”. PEM typically occurs with a delay of 12 to 48 hours after exertion and can last for days or weeks.
It can also lead to irreversible deterioration and a permanent change in the patient’s health in the long and short term. PEM can be mitigated by activity management techniques, often referred to as ‘pacing’. Patients are advised to minimize PEM episodes and prevent relapses by maintaining a balance between rest and activity.
The diagnosis of ME/CFS requires a careful differential diagnosis to explore alternative explanations for the symptoms, such as multiple sclerosis (MS) or major depression, but it is not a diagnosis of exclusion. It can occur alongside other conditions, and a number of comorbidities are even considered typical of ME/CFS. They are observed in many patients, probably due to as yet unexplained links in the pathomechanisms.

Additional symptoms

Deep exhaustion:
The fatigue associated with ME/CFS goes beyond normal tiredness. It is deep-seated, persistent and not easily relieved by rest.

Cognitive impairment:
ME/CFS can lead to difficulty concentrating, memory lapses and other cognitive challenges, often referred to as ‘brain fog’.

Sleep disorders:
People with ME/CFS often suffer from sleep disorders where restful sleep does not bring the expected relief, so they do not feel rested and refreshed when they wake up.

Postural orthostatic tachycardia syndrome (POTS):
This condition is associated with difficulties in maintaining normal blood pressure and heart rate when moving from lying to standing, resulting in symptoms such as dizziness, lightheadedness or fainting.
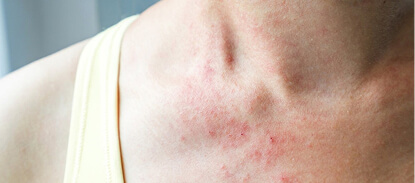
Mast cell activation syndrome (MCAS):
MCAS is an immunological disorder in which mast cells inappropriately and excessively release chemicals such as histamine, leading to symptoms in the skin, gastrointestinal tract, heart, respiratory tract and nervous system.
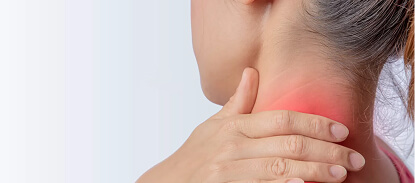
Pain:
Many people with ME/CFS suffer from pain, which can manifest itself in the form of severe muscle pain, joint pain and unbearable headaches, among other things.
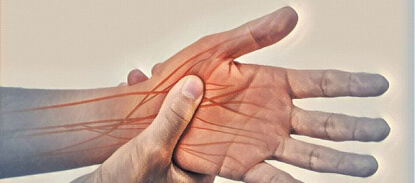
Small fiber neuropathy (SFN):
Small fiber neuropathy refers to the degeneration of small nerve fibers in the skin and eyes that transmit signals from the sensory and autonomic nervous system to the brain. SFN is often painful. Typical symptoms are sensitivity to touch and impaired temperature regulation.

Hypermobile Ehlers-Danlos syndrome (hEDS):
The main feature of hEDS is hypermobility of the joints caused by damaged connective tissue. Characteristic symptoms include joint pain and orthostatic intolerance. Many patients also suffer from chronic fatigue. Conversely, around 20% of people with ME/CFS fulfill the diagnostic criteria for hEDS.

Intolerance to environmental stimuli:
Most patients suffer from hypersensitivity or even intolerance to external stimuli such as sounds, light, smells and touch, making even simple activities such as looking at a screen for too long impossible. Due to these hypersensitivities, patients with very severe ME/CFS are confined to dark, quiet rooms.
We urgently support those affected by ME/CFS.
Life with ME/CFS
Together, we are on the path to a better life for ME/CFS patients.
Unfortunately, this takes time and does not happen overnight. ME/CFS patients do not simply wake up one day and return to their normal lives.
But there is hope, and we are here to fight for those who can no longer do so themselves. By funding more research and raising awareness, we will achieve our goal.
Step by step.
Join our cause
Every donation, no matter the size, fuels critical research and brings us one step closer to a cure.